Price gouging in prescription drugs was in the news lately. I got caught by it to a small extent.
I saw a dermatologist for a skin condition. The doctor said I had eczema, which is really a catch-all for skin problems of unknown causes. The doctor gave me a prescription. When I got to the pharmacy, the sales associate there asked me if I knew the prescription was really expensive. When I asked how expensive, she said the tube of cream was $230.
That was because I have a high deductible health plan. Instead of just paying a co-pay, I have to meet the annual deductible before the plan pays anything except for preventative care. That means both the office visit and the prescription were 100% on me.
$230 is the insurance company’s in-network negotiated price for that tube of cream. It’s the same price whether I fill it at Walmart, Target, or Costco. It’s a generic drug no less, and it’s on the insurance company’s formulary. Isn’t that crazy?
Unprompted, the pharmacy sales associate said they could hold it for 14 days for me to decide whether I want it. Apparently this happens often enough that they developed a procedure for it. Because I wanted to start my treatment right away, I just bit the bullet and paid $230.
The treatment is quite effective. If that’s the end of the story, I’m OK with paying $230 and putting my skin problem behind me. However, because the cause for eczema is unknown, there is also no cure. If the symptom returns, I’m very much against spending $230 on another generic tube of cream.
GoodRx
I learned that there is a website (and mobile app) called GoodRx. It’s not an online pharmacy. It gives you discount codes that you can take to a pharmacy near you for lower prices without going through insurance. Here’s the price GoodRx shows for my tube of cream:
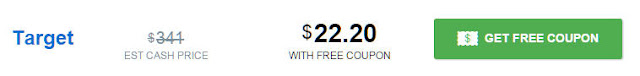
I don’t know how GoodRx is able to get it down to $22 when my insurance company is only able to negotiate to $230. Maybe the contract GoodRx found was signed before the manufacturer raised the price?
I haven’t tried it yet. So I don’t know whether this price from GoodRx will actually be honored. I will definitely try it if I need to refill my prescription.
Alternative Drug
If GoodRx doesn’t work, I will ask my doctor whether another drug will work just as effectively. There are usually alternatives. The doctor doesn’t necessarily know that one drug costs twice or even ten times as much as another.
My prescription benefit is provided by CVS Caremark. They have a website and a mobile app that can show you the cost of any drug covered by the plan. If the doctor gives me some alternatives I can look them up.
Lower Cost for All
The high deductible plan is working as intended. If I pay the same $15 co-pay on all generic drugs, I don’t have any incentive to seek out alternatives such as GoodRx or a different drug. By motivating the consumers, the high deductible plan lowers the cost for everyone. Yes I have to think more about my treatment options, but it’s good for the system overall.
[Photo credit: Flickr user ep_jhu]
Learn the Nuts and Bolts
I put everything I use to manage my money in a book. My Financial Toolbox guides you to a clear course of action.

Joseph Alexander says
Why not buy it without using insurance?
Greg Ray says
… and pay as much, or even more?
Jonathan says
There are a few strategies here.
Option 1: If in a perfect world you might be able to time when you need health care. If so, bias your health spending at the beginning of the year as doctors visits, not expensive prescriptions. Once you’ve met your deductible, your prescriptions will be less expensive.
Hypothetical with artificial numbers to illustrate point: you have a plan with $1,000 annual deductible, $15 copay on generics, 10% copay after deductible on doctor visits, and a need to visit two doctors, each billing $1k. If you visit the doctors early in the year and get the rx late in the year you’d pay $1000 + 100+15 = 1115. If you get the rx early in the year you’d pay $230 + 770 +23 + 100 = $1123. The savings aren’t materially different in this example, but in some circumstances they can be.
Option 2: something like GoodRx as you point out can work very well, especially with generics. One catch to using them. The amount you pay will not count towards your insurance annual deductible. In most (but not all) circumstances the savings can be significant and outweigh this disadvantage.
These strategies may often be out of touch with reality. But in certain circumstances — say you have the choice of timing some necessary but elective surgery — there’s a financial benefit to scheduling it at the beginning of the calendar year…
Mark Zoril says
My family, with two small children, has a high deductible plan. We live in Minnesota. We do not have an HSA – we pay for our costs out of our savings account. Our premium in 2013 was $229 a month. In 2016 it will be $580/month. I expect that it will probably end up around $800 to $1000 a month. We have had three significant health care events this year. My five year old broke her arm – I had the hiccups for 7 days (it was a bit scary – I was concerned it was going to be a long term thing) – and my wife had a medical event. Our total out of pocket costs this year will be around $13K or so with our premiums. Right now, our combined income is a bit below $100K.
Through this process we now know a lot more about how to shop for health care and also had to discuss costs, etc… In my view, most people should understand how to shop for and price health care costs. We shop for food, clothing, homes, insurance, household goods, and everything else. This should not be any different.
Harry Sit says
Mark – Please share your learning on how to shop for health care and discuss costs. As more people come out of the shield of a fixed co-pay, this knowledge is very valuable.
Richard Ericson says
As a physician, I can tell you that we have no way of knowing what a prescription will cost you. We have no mechanism to look up your specific medication on your plan at your pharmacy. I have been surprised many times when a generic medication available at Wal-Mart for $4 cost someone $100 at another pharmacy. You definitely have to communicate these issues to your doctor so they can offer alternatives.
Your statement that your cost will be the same at any pharmacy is not correct for the vast majority of patients on a high deductible plan. The price can vary dramatically from one pharmacy to another. I have had many patients save hundreds of dollars per month by switching pharmacies. Costco and Sam’s club are generally cheapest. Stores that have $4 generics are closely behind (Target, Wal-Mart and Raley’s/Bel Air here in California). I wouldn’t assume you can’t save money. Stop by the other stores with your insurance card and you might save significant amount of money each month.
Joe Blow says
As a physician you really could start by looking up GoodRx in front of patients and say that their insurance will either be close or much higher and mention they can choose to use either.
How much do you want to bet that your patients would love you for the savings?
It would probably take about 45 seconds to pull up the search in probably a 30 minute appointment.
Mark Zoril says
Per Joe Blow, if you do that for me I would tell everyone I knew what an amazing doc you were. I think that is a great idea. Maybe someone on your staff help your patients do this real quickly after their appointment.
Harry Sit says
It may be just how my insurance works on that specific drug. I tried pricing it at Costco and it’s the same to the penny as at Target if I use insurance.
Richard Ericson says
You’re expecting too much out of the appointment. We provide the Good Rx cards and I give patients a handout saying to let me know if cost is a problem. But you have to take ownership of your own healthcare. Don’t expect someone else to do the price shopping. It would be a complete waste of our time together for me to shop your medication for you. You are in the physician’s office for their training and expertise, not to show you how to surf websites.
Joe Blow says
I’ve used GoodRx numerous times and like you can’t make complete sense out of the discounts (although your discount is far larger than I’ve seen).
When you ask pharmacists to explain it they also can’t make sense of it.
From what I can gather it seems as though pharmaceuticals have been setting up programs to significantly discount drugs to the uninsured market. I’ve seen conflicting explanations on whether that is because:
a) Some government program that encouraged/obligated/something pharma to set up discounted drug programs for the uninsured.
b) The presence of insurance has created a giant price discrimination situation where insured aren’t price sensitive at all and uninsured/cash buyer are very price sensitive.
This thing has apparently evolved into a giant coupon/discounting system. GoodRx arrived at the right time to take these coupons aimed at the uninsured and repackage them for the masses.
An industry that heavily discounts on volume may have contributed to even larger discount coupons as GoodRx grew.
It appears GoodRx’s business model is in collecting what is known as dispensing fees?
Doug Hirsch says
Doug from GoodRx here….so, did you use one of our coupons? Pharmacy pricing defies all logic, and there are many inefficiencies which explain why we can find you a better price than your insurance co-pay. If you have any questions, let me know!
KD says
Doug, I have seen reluctance from patients to shop at different pharmacies for each prescription. Would GoodRx offer a service where a person puts in all their medications and GoodRx shows which store may offer the cheapest overall cost?
Martin Anderson says
Hi Doug,
I use GoodRX all the time. 🙂
How do you manage to get such good prices?
Martin Anderson says
GoodRX almost always works, and I also have no idea how it is that they manage to get such good prices. I found about them via a news story, possibly on 60 Minutes, about 3 years ago, and I now use them for every prescription.
Your savings are typical. For a bottle of Cleocin-T, which cost $15.00 when I was a kid, it’s now $85.00 without GoodRx, and $22.00 with.
Martin Anderson says
Also, make sure that at least one of your office visits every year or so is your preventative care check-up. Those visits are 100% free under the ACA, EVEN WITH A HIGH DEDUCTIBLE PLAN. But, if you don’t ask, you won’t receive that benefit.
Also, in my experience the very best way to buy health insurance is through a broker. Health insurance is one of the few instances where it is better to buy indirect. The broker, who receives a commission every month, can also be a good source to get issues remedied, since he or she has an incentive to keep you from switching to another carrier and typically has the inside numbers to reach the people who can get things done.
John says
We’ve had a high deductible plan for years. Initially it was much cheaper….now, not so much. However it did lead us to actually ask questions about how much something costs (drugs or a test). Amazing how much savings is available by asking. Doctors often have discount cards or rebate offers from the drug companies to dramatically lower our costs. It pays to ask the doctor when the prescription is written.
We’ll certainly try GoodRx. We’ve been calling around to a few pharmacies when we get a prescription. This might save us some time!
Thanks for the post.
John
Martin A. says
GoodRX appears to amalgate all of those discount cards that the doctor has.
If you really want to see something funny, check GoodRX while you’re still in the doctor’s office, and tell him how much the drugs cost. I’ve seen many an M.D. drop his or her jaw when I told them how much the drugs cost, and how much cheaper they can be had.
Bill says
Ironically, I had the very same experience just last week. The prescription to treat eczema was ~$230 because my deductible had not been met.
I work for a pharmaceutical company that makes generic topicals. The cost to actually make the medicine is only between $4 & $7 per unit. This is generics — Maddening!!!
Kevin M says
Have been using GoodRx for several years with my high deductible plan. Almost always saves lots of money over retail prices. My typical price is usually not much more than a typical copay would be (e.g., about $10 for generic), but of course it can vary widely.
Have had to move from one pharmacy to another though to get best price, and some chains, like Safeway and Target, no longer honor GoodRx coupons for certain controlled substances–I think maybe Schedule IV and lower. Other than this, the GoodRx coupon has always worked. Once they have it in their system, it seems to work like insurance, and I don’t have to show a coupon to get the discount on a refill.
Lately have been getting most prescriptions filled at Walgreen’s.
Sometimes best price is from an online supplier, but I’ve only used this for things I don’t have to sign for.
Kevin
sai says
Just came across a site to order meds from online and seems to be cheaper than store
healthwarehouse.com
Manuel says
If you have a high deductible plan and set up an HSA then you might be able to use GoodRX to pay for the prescriptions and then reimburse yourself from your tax-free HSA contributions (also for other IRS-approved medical, dental, and vision expenses).
Jason says
I have used GoodRx with success at Walgreens for a family member’s prescription. It was cheaper than the insurance price.
XY says
The issue with using GoodRX is that you can use EITHER your insurance OR a discount card. This means that in cases where it’s still very expensive even with GoodRX, you might be better off paying even more money on insurance so that at least your deductible gets used.
I just opted to pay $1600 out of pocket on Insurance instead of $400 with GoodRX so that I hit my 3k deductible. It’s going to get hit anyway, so might as well hit it sooner and have more things covered…
Marie says
Does the deductible refer to the drug or all medical expenses? I have a high priced deductible drug with lower monthly payments after that deductible I’d met. Very confused here.
- says
As to whether cash/GoodRX purchases can be applied to the deductible, YMMV and depends on your plan. It is true that (IME) you can’t apply both a goodrx coupon and insurance at the pharmacy point of sale; must choose one or the other. That said, some insurance plans have a manual claim form where you can submit a prescription receipt after paying a cash/coupon price. This won’t result in a payment if your deductible isn’t met, but it may result in a processed claim and EOB where the (coupon-discounted) price you paid is now counted toward the year’s deductible.
This form is usually specific to prescriptions and different from the one for general medical claims; it may come from the PBM/Rx subcontractor which might be a different entity or brand from the main insurance (eg CVS Caremark). In my case, it was an online form where you could attach the receipt, so it took about 5 minutes and not too difficult.
If you’re in this situation with an expensive drug and can track down the form, it’s probably worth venturing the attempt. Also note that independent/non-chain pharmacies, if you have them in your area, usually won’t accept goodrx type coupons, but may negotiate a cash price with you that gets close.